Authored by David Wilson-Wynne, Director or Innovare Dementia Consultancy
Published on 13 April 2026
Across health and social care, dementia remains one of the most discussed, researched, and strategised areas of practice. Yet despite decades of policy, frameworks, and well-intentioned models, many people living with a dementia continue to experience care that is structured around systems rather than around their own lives. The language has evolved – from task-based care to person-centred care – but the lived experience for many has not shifted as meaningfully as we might hope.
This raises a necessary and timely question: is person-led dementia care the change we now need?
The limits of “person-centred”
Person-centred care has been widely adopted as the gold standard in dementia care. It has rightly challenged the reduction of individuals to diagnoses and emphasised dignity, respect, and individuality. However, in practice, person-centred care can become diluted – reduced to a checklist, a care plan template, or a series of “preferences” documented but not truly enacted.
At its core, person-centred care often still positions the individual as a recipient of care that is designed and delivered by others. Even well-intentioned person-centred approaches may inadvertently position the person living with a dementia as a passive recipient of tailored services, rather than an active agent directing their own lives. Furthermore, the conceptual ambiguity surrounding person-centred care allow for interpretations that prioritise professional-led adaptations of care over true person-directed practice.
As a result, individuals may experience care that is personalised to them, but not led by them, reinforcing a subtle but important shift from agency to managed support.
This is not a failure of intent, but a limitation of the model.
What do we mean by person-led?
Person-led dementia care represents a fundamental shift – not just in practice, but in power.
It asks us to move beyond doing things for people or even with people, towards enabling people to direct their own lives in whatever ways remain possible to them. It recognises that living with a dementia does not remove a person’s right to agency, autonomy, or self-determination. Instead, it challenges us to find new ways to support these rights as cognitive changes occur.
Person-led care is not about independence in the traditional sense; it is about interdependence—a relational approach where support adapts to the person, rather than the person adapting to the system.
It means asking not only “what does this person need?” but “what matters to this person—and how do we follow their lead?”
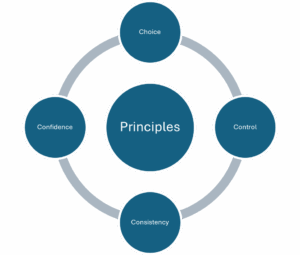
The principles of person-led care Choice, Control, Consistency, and Confidence—offer a clear and practical foundation for reshaping dementia care into something truly led by the individual (Wilson-Wynne, D. 2025).
Choice ensures that the person retains the right to make decisions about their everyday life, however big or small, recognising that preference and identity do not disappear with a diagnosis. Control moves this further, acknowledging the person as the primary decision-maker in their own life, rather than a passive recipient of care. Consistency provides the stability and familiarity that supports trust, reducing anxiety and enabling the person to navigate their world with greater ease. Finally, confidence underpins both the individual and the workforce—supporting people living with a dementia to feel secure in expressing themselves, while enabling staff to step back from rigid routines and trust in relational, responsive care. Together, these principles shift the focus from managing care to enabling lives to be lived on the person’s own terms.
Rebalancing power in care
At its heart, person-led care is about power. Who holds it? Who exercises it? And who benefits from it?
In many care environments, routines dominate. Mealtimes, medication rounds, staffing patterns, and organisational policies shape the day. While these structures may be necessary, they often leave little room for genuine choice or spontaneity. The result is a life that is safe and efficient, but not necessarily meaningful.
Person-led care requires us to critically examine these structures and ask whether they serve the person – or whether the person is being asked to fit within them.
For example:
- Can someone choose when to wake up, or is this dictated by staffing?
- Can someone decide what they want to eat in the moment, or only from a pre-set menu?
- Can someone opt out of “activities” altogether, without being labelled as disengaged?
These are not small questions. They go to the core of what it means to live a life with agency.
Language as a driver of change
 Language plays a crucial role in shaping how we think and act in dementia care (Wilson-Wynne, D. 2025) Terms such as “challenging behaviour”, “refusing”, or addressing people by need “wanderer” or “faller”, frame individuals in ways that can unintentionally diminish their personhood.
Language plays a crucial role in shaping how we think and act in dementia care (Wilson-Wynne, D. 2025) Terms such as “challenging behaviour”, “refusing”, or addressing people by need “wanderer” or “faller”, frame individuals in ways that can unintentionally diminish their personhood.
Person-led care demands a shift in language that reflects a shift in perspective. Instead of asking “what is wrong?”, we ask “what is being expressed?”. Instead of labelling someone as resistant, we explore whether the care being offered aligns with their wishes, identity, and lived experience.
This is not about semantics—it is about culture.
When we change our language, we begin to change our thinking. And when our thinking changes, so too can our practice.
Moving beyond activities to meaningful living
One of the most visible areas where person-led care can transform practice is in how we approach engagement.
Traditional models often rely on scheduled activities: bingo, crafts, music sessions. While these can be valuable, they risk becoming generic and disconnected from the individual’s identity. Participation is often encouraged—or even expected—regardless of personal relevance.
Person-led care shifts the focus from activities to meaningful living. It asks:
- What brings this person a sense of purpose?
- What has shaped their identity over time?
- How can everyday moments become opportunities for connection and expression?
Person-Led care asks us to view “identities” are something that evolves. As humans, we change our minds and this should be no different for people living with a dementia.
Importantly, person-led care also respects the right not to engage. Withdrawal, silence, or stillness are not necessarily problems to be solved—they may be expressions that require understanding.
Risk, rights, and dignity
A common tension in dementia care is the balance between safety and autonomy. Services are often risk-averse, prioritising protection over possibility. While safeguarding is essential, an overemphasis on risk can lead to overly restrictive practices that limit a person’s freedom and identity.
Person-led care reframes this balance. It recognises that a life without risk is not a life fully lived.
Supporting someone to make choices—even when those choices involve a degree of risk—is an expression of respect and dignity. It requires professionals to work alongside individuals and families, engaging in open conversations about what matters most.
This is not about abandoning responsibility; it is about sharing it.
The role of the workforce
Implementing person-led care is not simply a matter of changing policy—it requires a cultural shift across the workforce.
Staff need time, trust, and support to move away from task-driven models. They need to feel empowered to make decisions, to adapt routines, and to prioritise relationships over efficiency. This, in turn, requires leadership that values and models person-led principles.
Education also plays a key role. Training must go beyond knowledge of dementia as a condition, and instead focus on communication, relational practice, and reflective thinking. It should challenge assumptions and create space for staff to explore what it truly means to share power in care.
Designing environments that enable choice
The physical environment is often overlooked, yet it has a profound impact on how care is experienced.
Institutional layouts, long corridors, and centralised nurse stations can reinforce a sense of control and surveillance. In contrast, environments that are smaller in scale, more familiar, and easier to navigate can support autonomy and reduce distress.
Person-led design considers how spaces can enable choice:
- Can individuals move freely and safely?
- Are there recognisable landmarks that support orientation?
- Do private and communal spaces reflect real life, rather than institutional norms?
Design is not just about aesthetics—it is about enabling people to live in ways that feel natural and meaningful.
Person-Led Care is about evidencing how we have included individuals living with a dementia in the design of environments, as the true experts, their contribution should be an essential consideration for all care home providers for example.
Is this the change we need?
Person-led dementia care is not a new intervention or a programme to be implemented. It is a shift in mindset—a reimagining of what care can and should be.
It challenges us to move beyond comfort zones, to question long-standing practices, and to confront the imbalance of power that often exists in care settings. It asks us to see the person not as someone to be managed, but as someone to be followed.
The question is not whether we can adopt person-led care. The question is whether we are willing to make the changes required to truly embrace it.
As we look towards the future of dementia care, innovation must go beyond technology and infrastructure. It must reach into the heart of practice, into our relationships, our language, and our values.
Because ultimately, the change we need is not just in what we do—but in how we see.
And perhaps most importantly, in who we allow to lead.
Written by Dave Wilson-Wynne – March 2026
Director – Innovare Dementia Consultancy

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.

